
How HVAC Systems Help Reduce Potential COVID-19 Exposure:
As the economy begins to reopen and we return to our buildings, what role do building ventilation systems play in reducing our risks of infection? Infection via inhalation or contact with droplets is well understood at this point. Another potential exposure route being discussed is exposure via microdroplets, also called aerosols. The evidence for transmission via aerosols is currently incomplete. Until the potential for airborne viral transmission is better understood, the heating and cooling (HVAC) systems in buildings should be part of an overall strategy to limit the risk of indoor infections from COVID-19.
In the traditional infection control pyramid from the US Center for Disease Control and Prevention (CDC), the most effective controls, Elimination, and Substitution are currently not options. The next best option is Engineering Controls followed by Administrative Controls; the last resort is PPE. If used correctly, HVAC systems provide engineering controls to the spaces we occupy. Simulations [1] suggest that proper ventilation is effective in containment or minimizing [2] the virus in indoor environments.
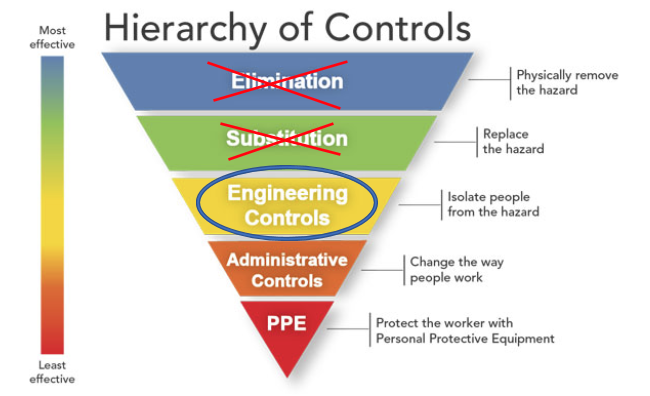
Figure 1. (Modified) Hierarchy of Controls for Protecting Workers from the U.S. CDC.
The virus travels in the form of droplets and aerosols (which are the droplets with the moisture evaporated and much smaller particles.) The moisture in droplets protects the virus and is also a larger particle that settles out of the air fairly quickly. Droplets are typically in the range of 10 micrometers (μm) and settle within 10 minutes. Aerosols can remain airborne from hours to days, however, they carry a lower concentration of the infectious virus.

Figure 2. Particle Settling Rates in Still Air.
Can the virus get pulled into the HVAC system and distributed throughout the building?
ASHRAE (the American Society of Heating, Ventilating, and Air-Conditioning Engineers) and the European counterpart, REHVA (the Federation of European Heating, Ventilation, and Air Conditioning Associations) have acknowledged this potential indoor airborne hazard and have compiled control measures. [3] [4]
Based on these guidance documents, the following practices are strongly recommended for commercial and public buildings (e.g. offices, schools, shopping areas, sports premises, etc.) where only occasional occupancy of infected persons is expected; hospital and healthcare facilities (usually with a larger concentration of infected people) have more extensive risks to manage and more engineering controls in place to control those risks.
ASHRAE Recommendations:
-
Do not recirculate air.
Increase outdoor air ventilation (disable demand-controlled ventilation and open outdoor air dampers to 100%) as indoor and outdoor conditions permit. There are energy use implications to not recirculating air and comfort may be compromised; however, it is more important to prevent contamination and protect public health than to guarantee thermal comfort.
-
Keep systems running longer hours (24/7 if possible).
Switch ventilation to a nominal speed at least 2 hours before the building usage time and switch to lower speed 2 hours after the building usage time. Do not switch ventilation off nights and weekends, but keep systems running at a slower speed. Keep toilet ventilation in operation 24/7 since transmission via fecal aerosols is possible.
-
Use high-efficiency filters.
Filtration can reduce the risk in recirculated air, however, not all filtration systems are equal. Many filters are only effective at removing larger particles and allow virus sized particles to pass through. High-efficiency filters can remove submicron-sized virus particles but can also reduce the performance of HVAC systems. Additionally, any gaps around the filter housing can render the filter useless. Ensure the system is well maintained and that modifications do not damage the system.
Recommendations with fair evidence for reducing exposure to occupants:
-
Temperature and humidity control.
It is not practical to use an HVAC system to create conditions necessary to inactivate the virus, however, maintaining relative humidity (RH) between 40-60% prevents the dehydration of nasal systems and mucous membranes in occupants which improves immunity to respiratory infections. It may also slow the dehydration of droplets allowing settling before aerosolization occurs.
-
Use personalized ventilation systems for certain high-risk tasks.
Workers having significant contact with the general public could benefit from a continual supply of fresh air.
-
Use portable, free-standing, high-efficiency particulate air (HEPA) filters.
Electrostatic filters are also considered to be effective. Ionizing filters are strongly discouraged due to the potential to generate ozone [8], a strong respiratory irritant. Increasing ventilation is more effective than portable filtration, however, if a portable device is employed, locating the device close to the occupant’s breathing zone.
-
Add duct or air handling unit mounted ultraviolet germicidal irradiation (UVGI) devices in high-density spaces.
The majority of modern UVGI lamps create UV-C energy at 254 nm wavelength, which is capable of inactivating the virus. The efficacy is dependent upon the UV dose and the susceptibility of the virus.
These recommendations supplement the personal hygiene and facility cleaning practices recommended by the WHO [7].
Is your building reopening soon? Healthy Building Science now offers Coronavirus Surface Testing and Cleaning Verification Audits for buildings moving toward reopening.
To get a bid for cleaning verification audit or testing for Coronavirus, SARS-CoV-2, COVID-19, please call 415-785-7986 or complete this online form today!
References
[1] Estimation [1] n of airborne viral emission: quanta emission rate of SARS-CoV-2 for infection risk assessmentGiorgio Buonanno, Luca Stabile, Lidia Morawska medRxiv 2020.04.12.20062828; DOI: https://doi.org/10.1101/2020.04.12.20062828 [2] L. Morawska, J.W. Tang, W. Bahnfleth, et al., How can airborne transmission of COVID-19 indoors be minimized?,Environment International (2020), DOI: https://doi.org/10.1016/j.envint.2020.105832 [3] American Society of Heating, Refrigeration and Air Conditioning Engineers (ASHRAE), ASHRAE Position Document on Infectious Aerosols, April 14, 2020.
https://www.ashrae.org/file%20library/about/position%20documents/pd_infectiousaerosols_2020.pdf [4] Baron, P. n.d. Generation and Behavior of Airborne Particles (Aerosols). Presentation published at CDC/NIOSH Topic Page: Aerosols, National Institute for Occupational Safety and Health, Centers for Disease Control and Prevention, Public Health Service, U.S. Department of Health and Human Services, Cincinnati, OH. www.cdc.gov/niosh/topics/aerosols/pdfs/Aerosol_101.pdf. [5] Federation of European Heating, Ventilation, and Air Conditioning Associations (REHVA). REHVA COVID-19 guidance document, How to operate and use building services to prevent the spread of the coronavirus disease (COVID-19) virus (SARS-CoV-2) in workplaces [7] World Health Organization (WHO). Getting your workplace ready for COVID-19.
https://www.who.int/docs/default-source/coronaviruse/getting-workplace-ready-for-covid-19.pdf?sfvrsn=359a81e7_6 [8] California Air Resources Board. Hazardous Ozone-Generating “Air Purifiers”.
https://ww2.arb.ca.gov/our-work/programs/air-cleaners-ozone-products/hazardous-ozone-generating-air-purifiers




[…] Have your HVAC system checked. Here’s what the experts at Healthy Building Science (HBS) recommend. […]